Why Do Implants Fail? What is Peri-implantitis? What Should Be Done?
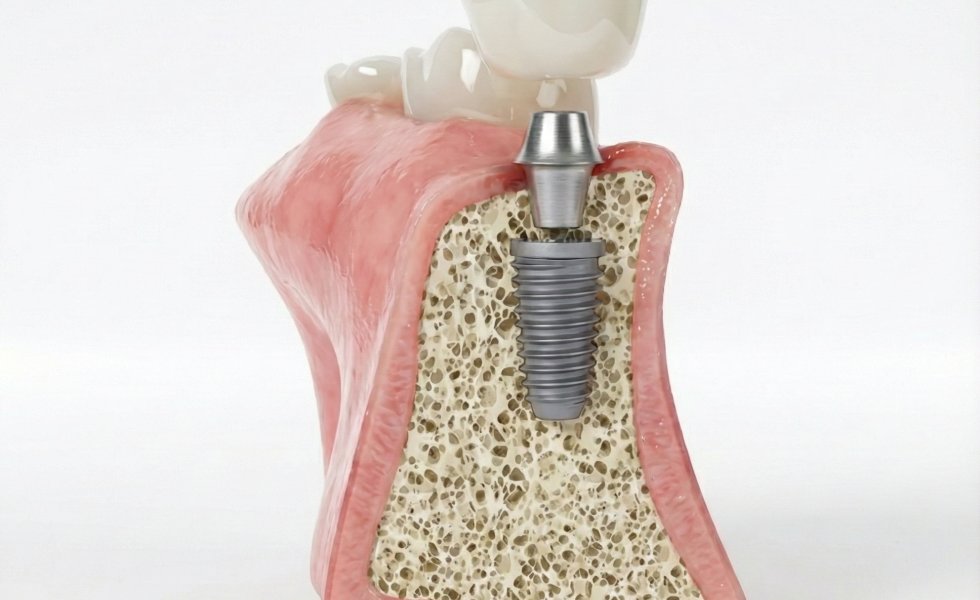
Peri-implantitis is a chronic infectious disease occurring in the tissues surrounding a dental implant, characterized by inflammation and bone loss. Simply put: your implant integrates with the bone like a tooth root; if bacteria accumulate in the surrounding gum and bone, it first leads to redness, bleeding, and if it progresses, to bone resorption and implant loosening.
Peri-implantitis is usually an advanced stage of untreated peri-implant mucositis. Patients often do not feel pain initially and may only notice bleeding during brushing, swelling, and bad breath. The radiographic finding of a crater-shaped bone loss around the implant is critical for diagnosis.
What should be done? The first step is correct diagnosis and patient education. First, the patient must understand that the area around the implant is even more sensitive than natural teeth and must adjust their daily care accordingly. Clinically, mechanical debridement (curettage, ultrasonic instruments) is used to clean the implant surface and surrounding tissues of bacterial plaque, and often antimicrobial agents (e.g., chlorhexidine mouthwashes or gels) are added.
For moderate and advanced cases, surgical treatment comes into play: by raising a flap, the granulation tissue is cleaned, the implant surface is decontaminated, and if necessary, regenerative surgery with bone grafts and membranes is applied. If the implant's stability is lost, sometimes complete removal of the implant may be necessary.
In summary: Peri-implantitis is not a condition where we can say "let's wait and see"; with early diagnosis, professional cleaning, surgery if needed, and regular follow-up, the lifespan of the implant can be extended. The patient's role is simple but vital: regular brushing, interdental cleaning, and not missing check-ups.
What is peri-implant mucositis?
Peri-implant mucositis is an inflammatory condition affecting the soft tissue (gum) around an implant, which has not yet caused bone loss. You can think of it as the equivalent of "gingivitis" for the implant surroundings. The most important point: if managed correctly, it is completely reversible, meaning catching the patient at this stage is golden.
Clinically, peri-implant mucositis presents as red, swollen gum around the implant that bleeds on brushing or probing. Radiographically, the bone level is normal, but biofilm/bacterial plaque accumulation is evident. In most cases, the patient does not complain of pain; this also causes the disease to be easily overlooked.
The basis of treatment lies in plaque control. First, the patient is explained in detail how to clean around the implant: a personalized routine is established using a soft-bristled toothbrush, interdental brushes, superfloss, or water irrigation devices. Then, mechanical debridement is performed in the clinic; meaning the bacterial plaque and soft deposits around the implant are removed with instruments that do not damage titanium. Short-term antiseptic mouthwash support can be provided if necessary.
If not managed well at this stage, peri-implant mucositis can progress to peri-implantitis, at which point bone loss, the need for surgery, and the risk of implant loss come into play. Therefore, the strategy must be clear for both the patient and the dentist: keeping the surrounding mucosa healthy is an integral part of the treatment, just as much as placing the implant.
Implant Loosening Failure, How Common is Peri-implantitis?
Peri-implantitis is a problem encountered more frequently today, parallel to the increasing number of implants. Although rates in the literature vary, different studies report peri-implantitis findings in approximately 15–25% of patients with implants. Simplifying it: we can think that roughly one in every 4–5 implant patients has a risk of encountering this problem at some point in their life.
This prevalence increases especially in the following groups:
-
Smoking patients,
-
Those with systemic diseases such as uncontrolled diabetes,
-
Those with a previous history of periodontal disease,
-
Patients who do not come for regular check-ups and neglect home care.
Another important point is the time factor. The first year after implant placement is usually the integration and prosthetic adaptation period. However, as years pass, especially after 5–10 years, the likelihood of bone loss and peri-implantitis increases. This tells us: an implant is not a "done and finished" deal; it is a treatment that requires lifelong care.
In daily practice, the most effective way to reduce the frequency of peri-implantitis is to correctly identify at-risk patients from the start, plan the treatment accordingly, and commit the patient to periodic check-ups in the long term. When discussing implant success, we must focus not only on surgical technique but also on patient compliance and long-term maintenance.
Implant Failure, What are the Causes of Peri-implantitis?
The primary cause of peri-implantitis, just like periodontal diseases, is bacterial biofilm (plaque) accumulation. However, due to the anatomy of the tissues around the implant and the characteristics of the implant surface, cleaning this biofilm is more difficult and inflammation can progress more rapidly.
We can summarize the main causes and risk factors as follows:
-
Inadequate oral hygiene: Plaque and calculus accumulating around the implant lead to gum inflammation and eventually bone loss.
-
Smoking: Nicotine reduces blood flow, slows healing, and increases susceptibility to infection.
-
History of periodontal disease: Individuals who have had gum disease before are in the high-risk group for peri-implantitis.
-
Systemic diseases: Especially uncontrolled diabetes, immunodeficiency conditions, and some medications make inflammation control difficult.
-
Poor implant planning and placement: Implants located in hard-to-clean areas, those subjected to excessive load, or those with inadequate bone support cause problems more quickly.
-
Unsuitable prosthesis design: Bridge and crown designs that are prone to food accumulation and make interdental cleaning difficult increase plaque retention.
-
Lack of regular check-ups: Bleeding and slight bone losses that could be detected early turn into advanced peri-implantitis if no check-up is performed.
In summary: Peri-implantitis is not the result of a single "mistake" but often a combination of plaque control + systemic
Features
- []
Comprehensive Dental Treatment
From routine checkups to advanced treatments, we offer a complete range of treatments to protect and beautify your health. Our personalized approach ensures that your special needs are carefully met.
All Treatments
- What Is A Dental Implant? Who Is It For And How Long Does It Take?
- Immedıate Implant Treatment In 1 Day
- All On Sıx Dental Implant Treatment
- What İs A Single Tooth İmplant?
- All-on-four Implant Treatment
- Implant Treatment Under General Anesthesıa
- Implant-supported Brıdge Treatment
- Why Do Dental Implants Faıl? Perı-ımplantıtıs Treatment
- Implant Placement Wıth Bone Graft
- Short Implants
- Guided Implant Surgery Treatment
- Sinus Lift Treatment
- Custom Subperıosteal Implant Treatment
- Implant Placement Wıth Ilıac Graft
- Zygomatic Implant Treatment