A Scientific Guide to Same-Day Immediate Implant
Missing teeth are not merely a cosmetic issue but a biomechanical problem affecting chewing, speech, and facial aesthetics. Although the thought of treatment "taking months" leaves many people hesitant, in suitable cases, the 1-day (immediate) implant approach allows for the implant to be placed in the same session as the tooth extraction and for aesthetics/function to be supported early with an out-of-occlusion temporary fixed prosthesis. This article combines clinical facts in patient-friendly language, summarizes the strengths and limitations in the literature, and explains step-by-step how a same-day planned treatment can be applied safely.
What is a 1-Day Immediate Implant?
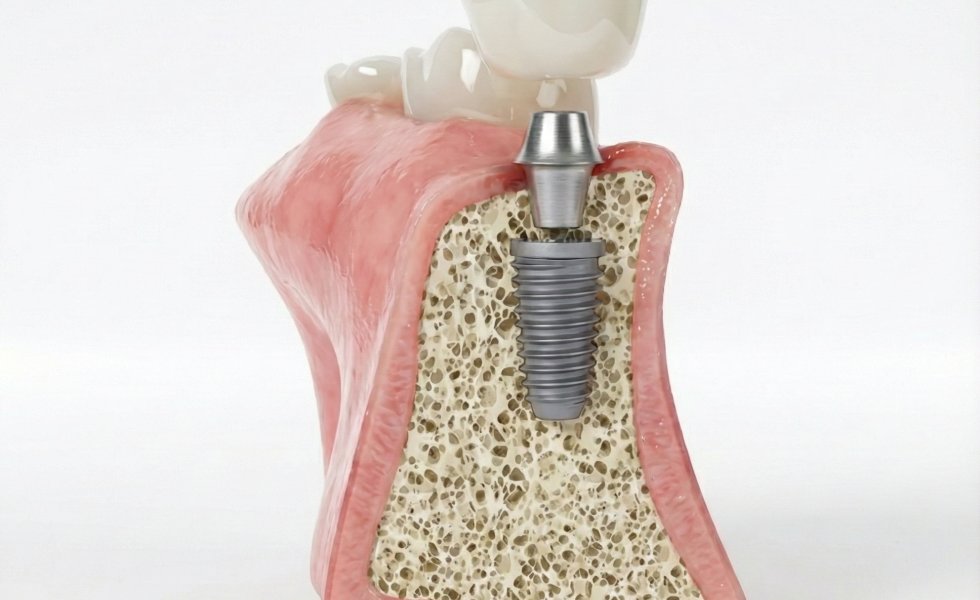
An immediate implant is the placement of the implant into the fresh socket immediately after tooth extraction. It is classified as Type 1 timing in the ITI classification. The goal is to reduce the total treatment time by utilizing the socket's existing anatomy, to preserve the crestal contour and soft tissue architecture as much as possible, and to offer the patient a socially acceptable temporary tooth on the same day. If adequate primary stability is achieved, the papilla and soft tissues can be shaped early with a screw-retained and out-of-occlusion temporary restoration.
In Which Situations Can a 1-Day Immediate Implant Be Applied?
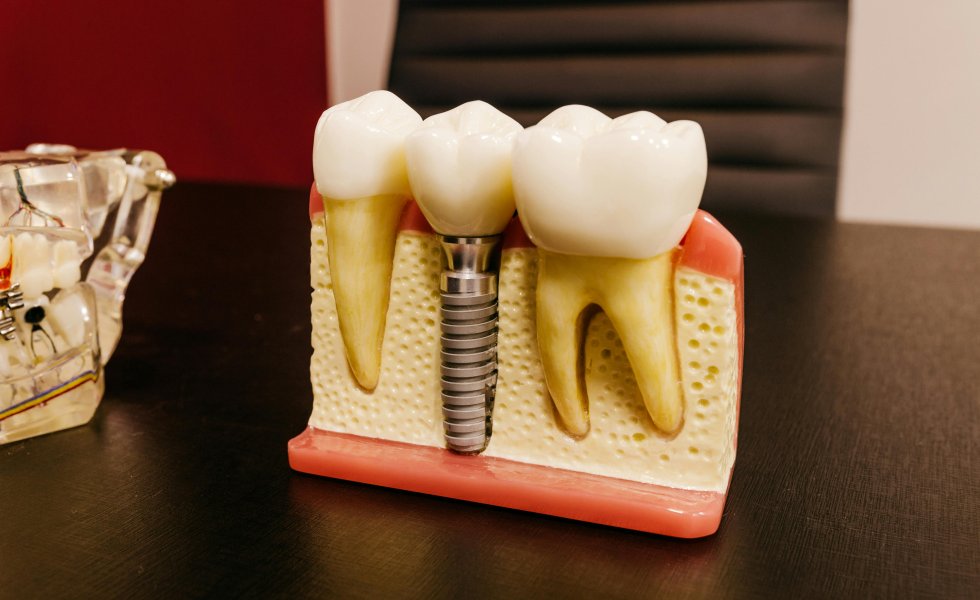
- Single Tooth Loss: Especially in the upper anterior region, the buccal wall is preserved by referencing the implant direction palatally/lingually.
-
Multiple Missing Teeth: Sufficient stability can be achieved in segmental gaps by utilizing apical/septal bone.
-
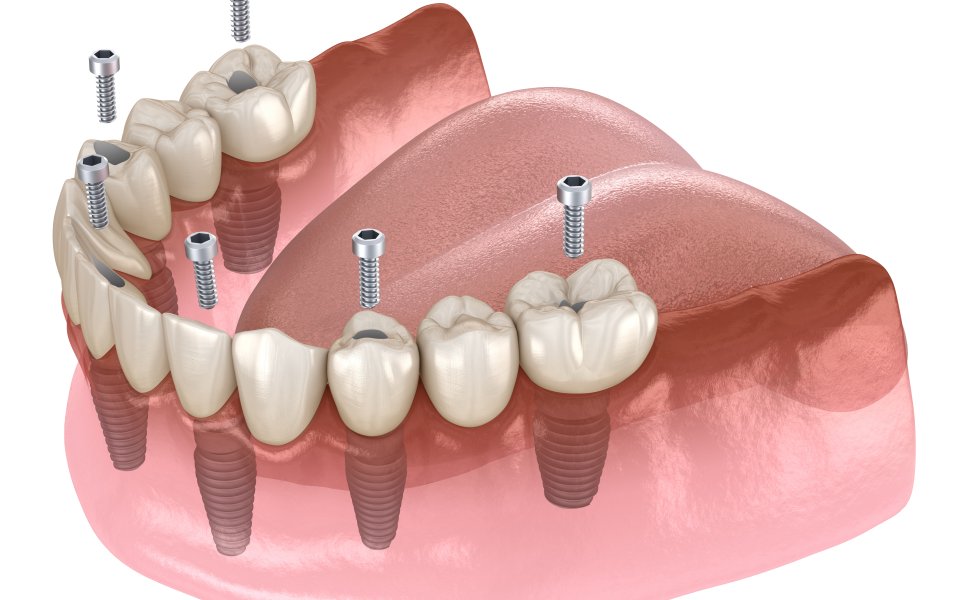
Complete Edentulism: With All-on-4 / All-on-6 protocols, a same-day fixed temporary bridge is possible thanks to tilted distal implants and planned occlusion.
The common denominator of these indications is the ability to achieve primary stability and the predictability of the soft/hard tissue biology.
Suitable Case Selection for 1-Day Immediate Implant: Indications and Contraindications
Preferred Conditions
-
Integrity of the buccal and lingual lamellae (especially the thickness and continuity of the buccal cortex).
-
≥3–5 mm of native bone apically and ≥35 Ncm torque; generally, an ISQ ≥60 range is considered safe.
-
Absence of acute purulent infection; applicability after meticulous debridement in chronic lesions.
-
Supporting soft tissue volume with a connective tissue graft in thin phenotypes.
-
Systemic conditions being under control, absence/minimal smoking, management of parafunctions.
Conditions Requiring Postponement/Alternative
-
Acute infection, fluctuant abscess, widespread alveolitis.
-
Combinations that increase aesthetic risk, such as advanced buccal defect, very thin phenotype, and a high smile line.
-
Bone quality/quantity that does not allow for primary stability.
-
Risk of uncontrolled early loading due to parafunction and opposing arch relationship.
What Does “1-Day Immediate Implant ” Mean?
The term "1 day" mostly encompasses two stages:
-
Extraction and implant placement,
-
Application of the out-of-occlusion temporary fixed prosthesis in the same session.
The purpose of this temporary restoration is to quickly meet the aesthetic need, support speech and social life, and guide the soft tissues into the desired profile. The permanent prosthesis is made after bone-implant fusion (osseointegration) is confirmed. In the mandible, this period can be planned as at least 5 weeks in most cases, and in the maxilla as at least 10 weeks; it is finalized by the physician according to individual healing and stability metrics.
Digital Planning and Guided Surgery in 1-Day Immediate Implant
- CBCT + intraoral scan (IOS) fusion; clarifies root form, buccal lamella thickness, apical bone length, and safe distances to neighboring anatomies (sinus, canal).
-
A digital surgical guide increases 3D accuracy, especially in the anterior region and with multiple implants.
-
A CAD/CAM temporary (screw-retained) restoration is applied the same day, managing papillary tissue with the emergence profile.
-
In complete edentulism, a virtual wax-up, vertical dimension, lip support, and phonetic mock-up improve the comfort and appearance of the same-day fixed temporary.
Step-by-Step Clinical Process
-
Atraumatic Extraction: The buccal wall is preserved through dissection at the PDL level, using the root section technique and controlled use of elevators.
-
Socket Debridement: Curettage of granulation tissue and copious saline irrigation; removal of infected/necrotic tissues.
-
Osteotomy Guidance: Palatal/lingual support in the anterior; aiming for 3–5 mm of apical engagement, away from the buccal wall.
-
Primary Stability: Tapered and aggressively threaded implant; targeting ≥35 Ncm torque and ISQ ≥60 with an under-preparation approach.
-
3D Position: Platform slightly palatal relative to the buccal crest; ~3 mm apical to the cervical reference. Attempt to maintain ≥2 mm buccal bone thickness.
-
"Jumping Gap" Management: If the implant-wall gap is ≥1–2 mm, use particulate graft (in most cases, slow-resorbing xenograft) and collagen plug; a membrane is often not needed with an intact wall.
-
Soft Tissue Optimization: Buccal profile and coloration are supported with a connective tissue graft in thin phenotypes.
-
Temporary Restoration: Screw-retained, completely out-of-occlusion; eccentric and vertical contacts are removed. If stability is insufficient, a cover screw and delayed loading are preferred.
-
Medication and Care: Protocol-appropriate antibiotics, 0.12–0.2% chlorhexidine, analgesics; avoidance of smoking and trauma.
-
Follow-ups: Soft tissue at 2–3 weeks; temporary profile adjustment at
Features
- []
Comprehensive Dental Treatment
From routine checkups to advanced treatments, we offer a complete range of treatments to protect and beautify your health. Our personalized approach ensures that your special needs are carefully met.
Areas We Serve
Immedıate Implant Treatment In 1 Day – Areas We Serve
We deliver chairside implant and dental treatments across every district of Istanbul with local expert teams.
Sultanbeyli Immediately Implant Treatment
In Sultanbeyli, get your missing teeth instantly with 1 Günde Hemen İmplant (Immediate) treatment! At İmplanttr, we offer safe and permanent smiles.
- Treatment is completed in a single day.
- The waiting period and gap after tooth loss are eliminated.
- Aesthetics and function are quickly restored.
ÇEKMERKÖY Immediately IMPLANT TREATMENT
Missing teeth? Get a permanent solution with same-day immediate implants in Çekmeköy. At İmplanttr, we give you a new smile in just one day.
- Saves time by significantly shortening treatment duration.
- Psychological distress and social reservations after tooth loss are minimized.
- Reduces number of procedures with extraction and implant in one session.
Samandıra Immediately Implant Treatment
Missing teeth? In Samandıra, get a permanent solution with 1 Günde Hemen İmplant (Immediate Treatment). At İmplanttr, we restore your smile the same day.
- Treatment is completed in a single day, saving time.
- The gap after tooth loss is filled immediately, preserving aesthetics.
- Chewing function is quickly regained, preventing dietary disruption.
Yenidoğan Immediately Implant Treatment
Yenidogan Implant Treatment in your area! With İmplanttr, get immediate implant treatment in 1 day. Say goodbye to missing teeth, hello to your new smile.
- Patient comfort increases as treatment time is significantly shortened.
- Bone loss in the extraction socket is minimized, preserving natural structure.
- Teeth are obtained instantly without loss of aesthetics or function.
All Treatments
- What Is A Dental Implant? Who Is It For And How Long Does It Take?
- Immedıate Implant Treatment In 1 Day
- All On Sıx Dental Implant Treatment
- What İs A Single Tooth İmplant?
- All-on-four Implant Treatment
- Implant Treatment Under General Anesthesıa
- Implant-supported Brıdge Treatment
- Why Do Dental Implants Faıl? Perı-ımplantıtıs Treatment
- Implant Placement Wıth Bone Graft
- Short Implants
- Guided Implant Surgery Treatment
- Sinus Lift Treatment
- Custom Subperıosteal Implant Treatment
- Implant Placement Wıth Ilıac Graft
- Zygomatic Implant Treatment