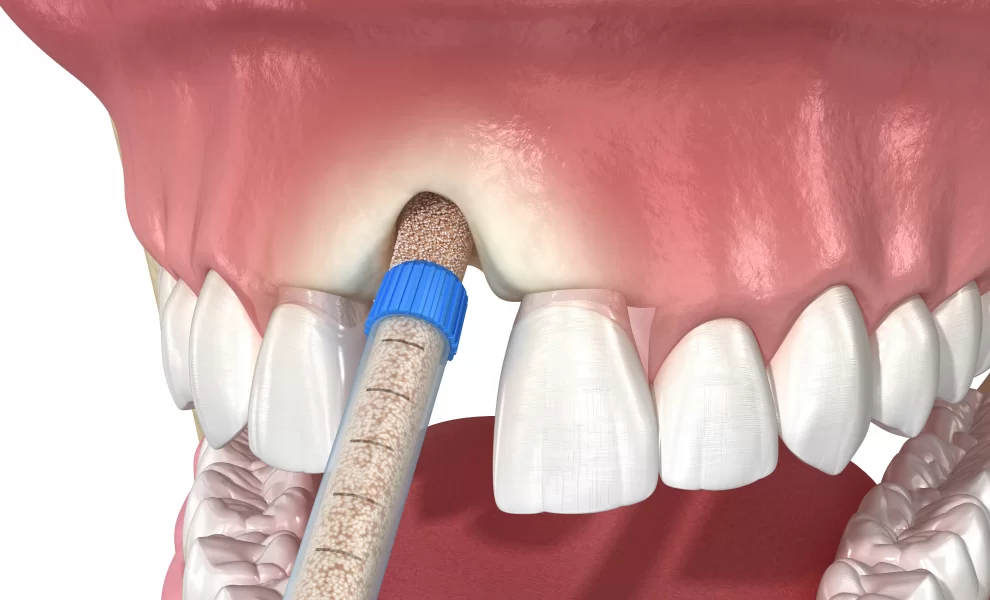
Bone Grafting For Dental Implants
Bone grafting for dental implants rebuilds the jawbone so implants can stay stable and last for many years. After tooth loss, the bone shrinks and may become too thin or narrow for a safe implant. A graft fills and reshapes the defect, but success depends on several linked factors: a clean, infection-free site, tight gum closure, enough protected space, complete stability and strong blood supply. With tools like membranes, tent screws, fixation and decortication, surgeons guide the body’s own healing and bone formation step by step. When all these keys work together, a weak or resorbed jaw can become a strong, long-term foundation for natural-looking implant teeth.
Bone Grafting for Dental Implants: The Hidden Foundation of a Strong Smile
When people think about dental implants, they usually picture the white ceramic crown that shows when they smile. In reality, the long-term success of an implant depends on what you cannot see: the quality and volume of the jawbone underneath.
After a tooth is removed, the jawbone in that area naturally starts to shrink. Over the first few years, the bone can lose a significant amount of height and width. Without enough strong bone, an implant cannot hold, stay stable or last for many years.
To prevent this “disappearing bone” problem, dentists use a procedure called bone grafting. But bone grafting is not just “filling a hole with bone powder”. It is a delicate biological process that must be planned and protected carefully.
This article explains the main keys to successful bone grafting and how they help your jaw become a solid base for future implants.
Bone Grafting Is Like Opening a Combination Safe
Bone grafting is not magic; it is controlled healing. You can think of it like trying to open a combination safe. If there are 11 numbers in the code and you only get 6 or 7 of them right, the safe will not open.
Bone grafting works the same way. If one or more of the “keys” to healing are missing – for example, good blood supply, stability or a clean environment – the graft may not turn into strong bone.
Below are the most important keys your surgeon must control for a predictable result.
Key 1: No Infection – Keeping the Area Clean
The mouth is full of bacteria, but for a bone graft to work, the surgical area has to be as clean as possible.
Infection creates a very aggressive, acidic environment around the bone. In such conditions, bone and graft particles can start to dissolve instead of healing and hardening. If germs get into the graft, they can destroy it before the body has a chance to turn it into real bone.
That’s why your dentist will:
-
Clean the area thoroughly
-
Remove infected tissue or old, failing teeth or fillings
-
Sometimes mix antibiotics with the graft material to protect it in the first days, when it has no blood supply of its own
Key 2: A Good Soft Tissue Seal – Closing the Gums Properly
Imagine trying to grow a plant while its roots are constantly exposed to wind and dirt. It would dry out and die. Bone grafts are similar: they must be fully covered and protected by the gums.
For this reason, primary soft tissue closure is essential. This means the gums are brought together and stitched over the graft so that no graft or membrane is left open to the mouth. If the wound opens during healing, bacteria and saliva can reach the graft and cause it to fail.
To prevent this, your surgeon may:
-
Release and gently stretch the gum tissue so it can close without tension
-
Use special flap or tunnelling techniques to allow the gums to slide over a larger grafted area comfortably
Key 3: Space Maintenance – Creating Room for Bone to Grow
Bone cannot grow where there is no space. If the soft tissue collapses into the defect, that space will be filled with gum tissue instead of new bone.
To stop this from happening, your dentist uses space-maintaining techniques, such as:
-
Barrier membranes: Thin sheets that cover the graft and stop soft tissue from growing into it
-
Tent screws or pins: Small screws that hold the membrane up, like poles of a tent, so the bone can form underneath
-
Slight overfilling (“barrier by bulk”): Adding a little extra graft so that, even if the outer layer remodels, the inner part still becomes solid bone
Key 4: Stability – “Don’t Shake the Jelly”
When you break an arm, it is put in a cast. If the bones keep moving, they can’t join. Bone grafts also hate movement.
Even very small micromovements can stop new bone from forming and instead lead to soft scar tissue. The graft must stay completely still while blood vessels and bone cells grow into it.
To achieve this, your surgeon might use:
-
Fixation screws to lock a block of bone onto the jaw
-
Tacks or pins to hold a membrane tightly in place
-
Fixed temporary teeth instead of a removable denture that presses on the graft when you chew
Key 5: Activating Healing – The Regional Acceleratory Phenomenon (RAP)
Bone is a living tissue that reacts strongly to controlled injury. When the bone is stimulated, the body sends extra healing cells and blood flow to that region. This is known as the Regional Acceleratory Phenomenon (RAP).
To trigger this, your surgeon often makes small holes in the outer layer of your natural bone (decortication) before placing the graft. This:
-
“Wakes up” the bone and speeds up the healing response
-
Opens channels for blood vessels and bone-forming cells (osteoblasts) to enter the graft quickly
Key 6: Blood Supply – The Lifeline of the Graft
Placing bone material in a space is not enough. Without blood, there is no life and no new bone.
Soft tissue grows fast; bone grows slowly. There is always a race between the two. By opening the base bone and triggering RAP, blood vessels from your own jawbone grow into the graft. These vessels carry:
-
Oxygen and nutrients
-
Bone-building cells
-
Growth factors needed for proper bone formation
When this happens early and strongly enough, bone wins the race and fills the defect before soft tissue takes over.
Materials Used in Bone Grafting
Your surgeon can use different types of graft material, sometimes in combination:
-
Autograft: Bone taken from another area of your own body or jaw. This is often considered the gold standard, as it contains your own living cells and natural growth factors.
-
Allograft: Processed donor bone from a human source. It acts as a scaffold, helping your body to replace it with its own bone over time.
-
Alloplast (synthetic grafts): Man-made materials (such as certain ceramics) that mainly work as space fillers and support.
-
Growth factors / PRP: Platelet-Rich Plasma taken from your own blood, rich in healing proteins that can speed up soft tissue repair and support blood vessel growth around the graft.
In Summary
Bone grafting for dental implants is a carefully planned procedure that rebuilds the jaw so it can hold implants safely and for the long term. Success does not depend on one factor alone. It is the result of:
-
A clean, infection-free site
-
Gums that close and seal the area
-
Enough space for bone to grow
-
A completely stable graft
-
Activated healing (RAP)
-
Strong blood supply from your own jawbone
When all these keys are respected, a “vanishing” jawbone can be transformed into a strong, stable foundation for dental implants and a confident, lasting smile.

M. İhsan GÜRSOY / Diş Hekimi
Author