Implant Terms In Dentıstry: Your Guıde To The Jargon
Clear and consistent terminology ensures clinicians communicate accurately with colleagues, technicians, and most importantly, patients. #İmplanttr
Dental Implant Terminology
Implant dentistry is a highly systematic and structured field; the language and terms used directly reflect this structure. Clear and consistent terminology enables clinicians to communicate accurately and completely with each other, with technicians, and most importantly, with patients. Therefore, understanding basic and advanced implant terms is not merely an academic interest; it is a necessity that determines the quality of diagnosis, treatment planning, and long-term care. This text aims to summarize the most frequently used terms in implant dentistry within a systematic and practical framework.
Basic components: implant, abutment, and prosthesis
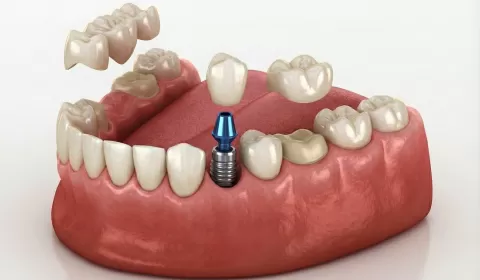
At the core of implant dentistry are three main components: the implant, the abutment, and the prosthesis.
The dental implant (fixture or endosseous implant) is the part placed inside the bone that acts as an artificial root. It is typically made from titanium or titanium alloy; in some cases, zirconia implants are also preferred.
The abutment, which is connected onto the implant, is the part that provides the mechanical connection between the implant and the prosthesis. Abutments can be prefabricated, custom-milled, straight or angled, screw-retained, or cement-retained designs. Abutment selection directly influences the emergence profile, soft tissue support, and direction of load transfer.
The visible part in the mouth is the prosthesis or implant-supported restoration. This can be a single crown, a bridge, an overdenture, or a full-arch fixed restoration. The term "implant crown" describes the prosthetic tooth that is attached to the implant via the abutment.
Osseointegration and the bone-implant interface
One of the most important terms in implant dentistry is osseointegration. This refers to the presence of a direct, stable, and fiber-free contact at the microscopic level between living bone and the implant surface. Thanks to this biological connection, the implant can be functionally loaded in an immobile and pain-free manner.
The area where the bone joins the implant is called the bone-implant interface. Terms such as bone-to-implant contact percentage, crestal bone level, and marginal bone loss describe how well this interface is maintained over time. These parameters play a critical role in success criteria and long-term follow-up assessments.
Implant design: macro structure and micro structure
The macro designs of implant bodies are clearly distinguished in the terminology used. The most common forms are cylindrical and tapered implants. The external shape is the main factor determining primary stability and how functional forces are distributed within the bone.
Most implants have a threaded design. The screw-like spirals running along the surface are described by terms such as pitch, thread depth, and thread angle. Thread geometry influences how the implant advances into the bone and how forces are transferred during chewing loads.
At the micro level, the concepts of surface topography and microstructure are used. The implant surface can be machined, acid-etched, sandblasted, coated, or nanostructured. Terms like "moderately rough surface" and "hydrophilic surface" describe surface treatments aimed at accelerating osseointegration and improving healing.
Connection types and platform concepts
The implant-abutment connection defines how the abutment is attached to the implant. Among the most commonly used connection types are external hexagon, internal hexagon, and internal conical (morse taper) systems.
-
External Hexagon: The hexagonal structure is located on top of the implant platform.
-
Internal Hexagon / Internal Conical: The connection element is positioned inside the implant body and generally aims to provide better orientation and reduce micro-leakage.
Two important terms frequently heard in modern implantology are platform matching and platform switching.
-
In platform matching, the abutment diameter is equal to the implant platform.
-
In platform switching, the abutment is narrower than the implant platform, creating a horizontal step. This approach is associated with crestal bone preservation and enhanced soft tissue stability.
Timing-related terms: placement and loading
When the implant is placed and when it is loaded with a prosthesis are expressed with specific terms:
-
Immediate Implant Placement: Placement of the implant into the fresh extraction socket during the same appointment as the tooth extraction.
-
Early / Delayed Placement: Application of the implant after allowing the socket to heal for a certain period (weeks–months).
In terms of loading:
-
Immediate Loading: The implant is brought into function with a temporary or final prosthesis in a very short time – usually within the first 48 hours.
-
Early Loading: Loading performed within a few weeks.
-
Conventional Loading: Loading after an average waiting period of three months in the mandible and four–six months in the maxilla.
Timing selection is made by evaluating primary stability, bone quality, occlusal loads, and the overall risk profile.
Surgical terms: one-stage, two-stage, and flap approaches
One-stage surgery is a protocol where the healing abutment is also placed and left trans-mucosal along with the implant placement; it does not require a second uncovering surgery.
In two-stage surgery, the implant remains completely submerged under the mucosa during the healing period; it is later exposed via a second surgery for abutment connection.
Flap design is also an important part of the terminology:
-
Flapless method: The implant is placed via a punch or minimal incision without raising a full mucoperiosteal flap.
-
Flap method: The mucosa and periosteum are raised to expose the bone.
Terms used in these approaches include crestal incision, vertical releasing incision, full-thickness flap, and partial-thickness flap.
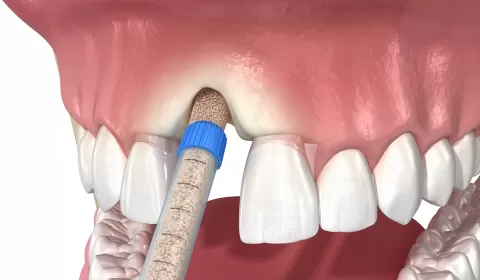
Bone quality, quantity, and anatomical references
One of the most frequently referenced classifications in planning is the Misch bone density classification:
-
D1: Very dense cortical bone
-
D2: Combination of thick cortical and dense trabecular bone
-
D3: Thin cortical and looser trabecular bone
-
D4: Soft, thin trabecular bone
Terms like "D2 bone" or "D3 bone" provide quick information about the expected stability and drilling protocol.
Available bone is expressed by the height, width, and length in the area planned for the implant. The terminology also uses concepts such as crestal width, vertical bone deficiency, buccal undercut, and sinus pneumatization.
Anatomical structures like the inferior alveolar nerve, mental foramen, maxillary sinus, and incisive canal are fundamental reference points in surgical planning.
Prosthetic terms: retention, support, and design
The most commonly used terms in the restorative phase are:
-
Screw-retained restoration: The prosthesis is attached to the implant or abutment with a screw; the restoration has a channel for screw access.
-
Cement-retained restoration: The crown or bridge is cemented onto the abutment.
In

M. İhsan GÜRSOY
Author